
Osteochondrosis is a form of degenerative disease of joints and intervertebral discs. Osteochondrosis damages the cartilage tissue of the discs. As a result, the disc hardens and shrinks, loses its protective properties and causes severe pain.
Cervical osteochondrosis is a progressive degenerative-dystrophic process that causes degeneration, deformation and destruction of the intervertebral discs of the cervical region. Loss of shock-absorbing cartilage causes pain due to both impaction of the joint surfaces (spondyloarthrosis) and compression of the nerve roots of the spinal cord.
In the absence of timely treatment, ossification of the spine is possible due to loss of its natural flexibility, violation of blood supply to the brain, deterioration of nerve conduction in those parts of the body that innervate the roots of the cervical spine.
Pathology can develop both independently and as part of a general damage to the spine, which includes the thoracic, lumbar and sacral areas.
General information about cervical osteochondrosis
It is believed that osteochondrosis of the cervical spine is more common than in other departments. In fact, this is not so - dystrophic events develop equally at all points of maximum load - in the area of the main curves of the spinal column (the lower the section, the greater the load on it). However, the symptoms of cervical osteochondrosis are more pronounced, so it seems to be more common. This is due to the high mobility of the neck vertebrae, which at the same time hold the head, as well as the peculiarity of the location of the roots of the spinal cord.
Note!According to statistics, the disease affects more than 60% of middle-aged and elderly people. However, recently there has been a rejuvenation of the pathological process - the pathology occurs in young people and even adolescents. This is due to the general computerization of learning and work, as well as a decrease in physical activity and a deterioration in the quality of nutrition.
Considering the age of the audience, 2 forms of cervical osteochondrosis can be distinguished - physiological and pathological.
physiological processAssociated with the natural aging of the body, when the symptoms of the disease are the result of the gradual wear and tear of the intervertebral discs. The process takes place under the influence of the endocrine system and is the result of menopause changes. The destruction of cartilaginous structures starts from the center of the intervertebral disc and is accompanied by the gradual replacement of cartilaginous tissue with fibrous tissue. The pathology is irreversible, but it can be compensated with special medicines.
pathological processAssociated with pathological destructive changes in the body - immune, dystrophic, inflammatory, metabolic. First of all, pericartilaginous tissues are involved - salt deposits appear on bone structures, nerve roots are inflamed, skeletal muscle atrophy or hypertonicity occurs, which causes blood circulation disorders in the head-neck-chest area. With timely diagnosis, the pathology is curable and ends with the full restoration of the healthy function of organs and tissues.
Stages of cervical osteochondrosis and their symptoms
There are 4 main stages of the pathological process:
- Stage 1 - expressed by slight discomfort and muscle tension in the affected area, cartilage discs lose stability;
- Stage 2 - there is local pain, especially when moving the head. The intervertebral discs are deformed, the fibrous ring begins to collapse, the distance between the vertebrae decreases;
- Stage 3 - pain intensifies and becomes constant, movements are limited. Turning the head can cause vertigo attacks, nausea, impaired blood supply to the brain causes general lethargy, fatigue, impaired concentration, cartilage thins, vertebrae close, the fibrous ring is completely destroyed with the risk of intervertebral hernia development;
- 4th stage - pain syndrome completely immobilizes the neck; The blood circulation of the brain is impaired and requires constant medical assistance; The vertebrae begin to grow together.
Cervical osteochondrosis: signs, symptoms, pathology treatment
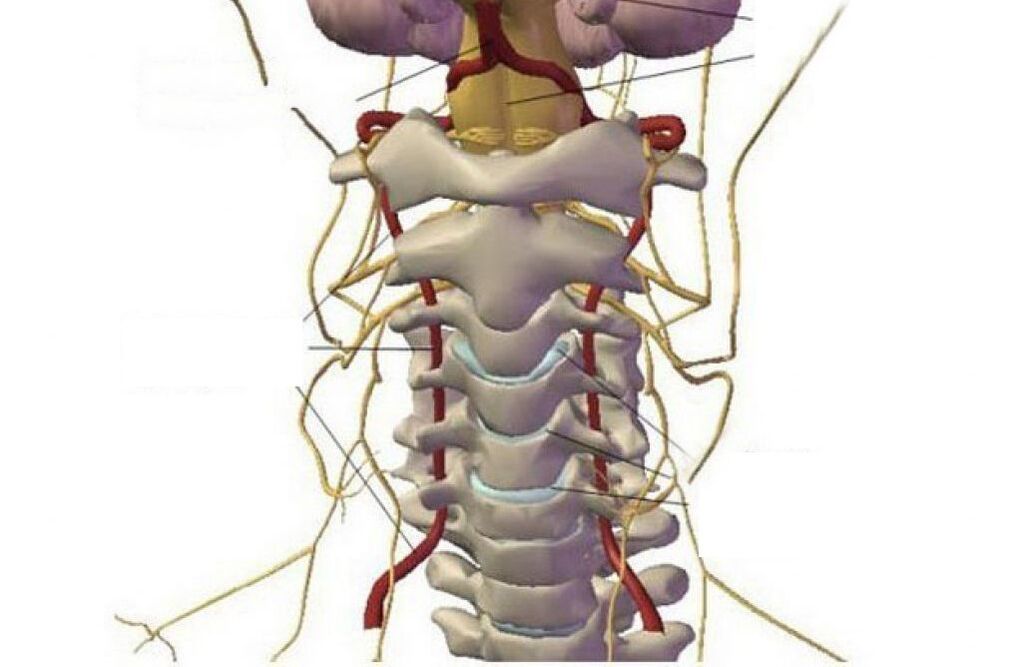
In the first stage, osteochondrosis is asymptomatic. During the development of the disease, a distinctive feature is the presence of painful or uncomfortable sensations in the head, neck and chest, less often in the upper limbs.
All possible symptoms can be conventionally attributed to 4 types of syndrome: heart, spine, radicular (nerve) and vertebral artery syndrome (with vascular disorders).
Spine syndrome:
- Neck cramping when turning/tilting the head;
- As the disease progresses, pain and difficulty in movement appear;
- Morphological structural disorders in the vertebral body and intervertebral space (visible on X-ray).
Heart syndrome:
- shortness of breath, weakness;
- feeling of incomplete inspiration, lack of air;
- Spontaneous events of the cardiovascular system - angina pectoris, retrosternal pain, burning;
Radicular syndrome:
- numbness of the tongue, shoulders, fingers, nape of the neck;
- difficulty swallowing;
- discomfort in the area between the shoulder blades;
- Headache in the occiput and forehead.
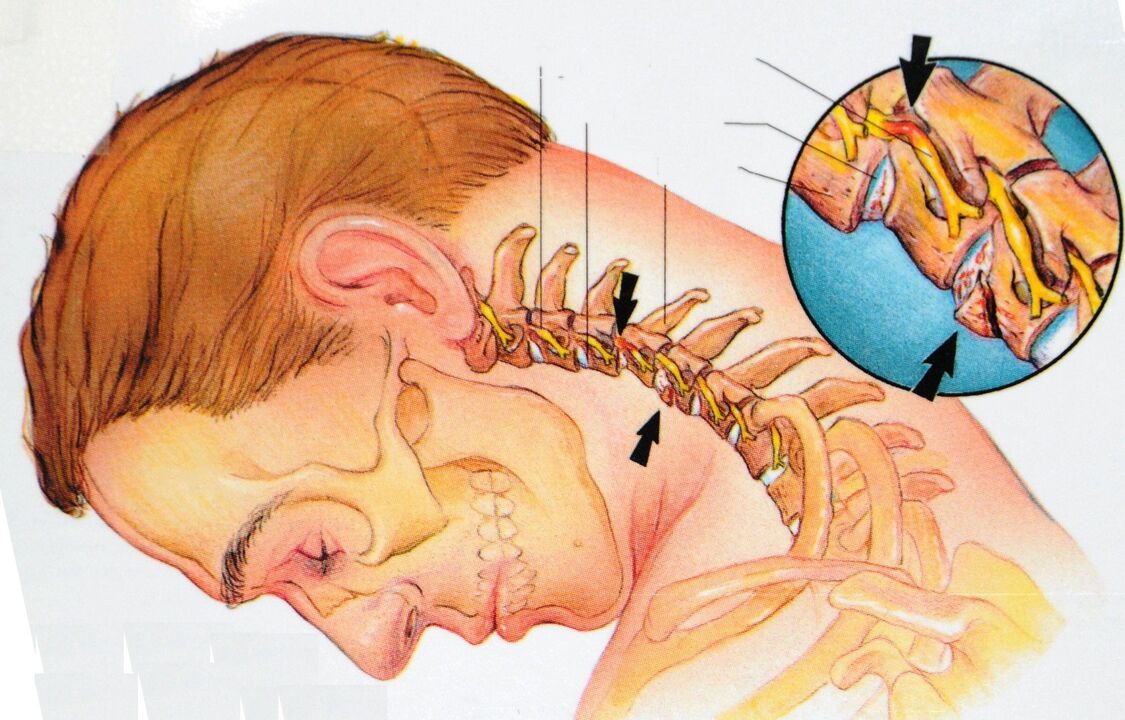
Vertebral artery syndrome:
- unreasonable jumps in blood pressure;
- dizziness, before losing consciousness;
- tinnitus, sensation of cotton wool in the head;
- temporary one-sided blindness, "flying" in the eyes;
- periodic attacks of nausea, especially when moving the head;
- Headache - mainly in the back of the head, also migraine;
- Drowsiness, decreased performance, memory, concentration, depression.
Attention!All these syndromes must be combined with each other. Absence of symptoms of one of them can be a reason for differential diagnosis with other groups.
Causes of cervical osteochondrosis
Dystrophic events in the region of the cervical spine are related to the vertical position of the skeleton and the specific distribution of static and dynamic loads, which largely depends on the prevailing posture and the degree of skeletal muscle development.
- Lack of movement - which does not develop - decreases: muscles weaken, tissues are destroyed;
- Incorrect static postures - muscle clamps cause blood circulation disorders with subsequent tissue dystrophy;
- Lack of nutrition or an unbalanced diet - the body must receive everything necessary to build and renew skeletal bone and cartilage structures, to maintain muscle tone;
- obesity, overweight, carrying heavy loads - the load on skeletal structures increases;
- constant nervous tension and nervous stress;
- Hypothermia of the cervical region - "cold", "bloated" - provokes hidden inflammatory processes;
- The presence of autoimmune diseases together with cartilage leads to its premature destruction;
- Endocrine pathologies disrupt mineral metabolism, reduce the absorption of calcium, silicon, phosphorus and other elements of bone and cartilage tissue;
- neck injuries;
- Congenital anomalies of the spine and surrounding muscles.
Diagnosis of cervical osteochondrosis
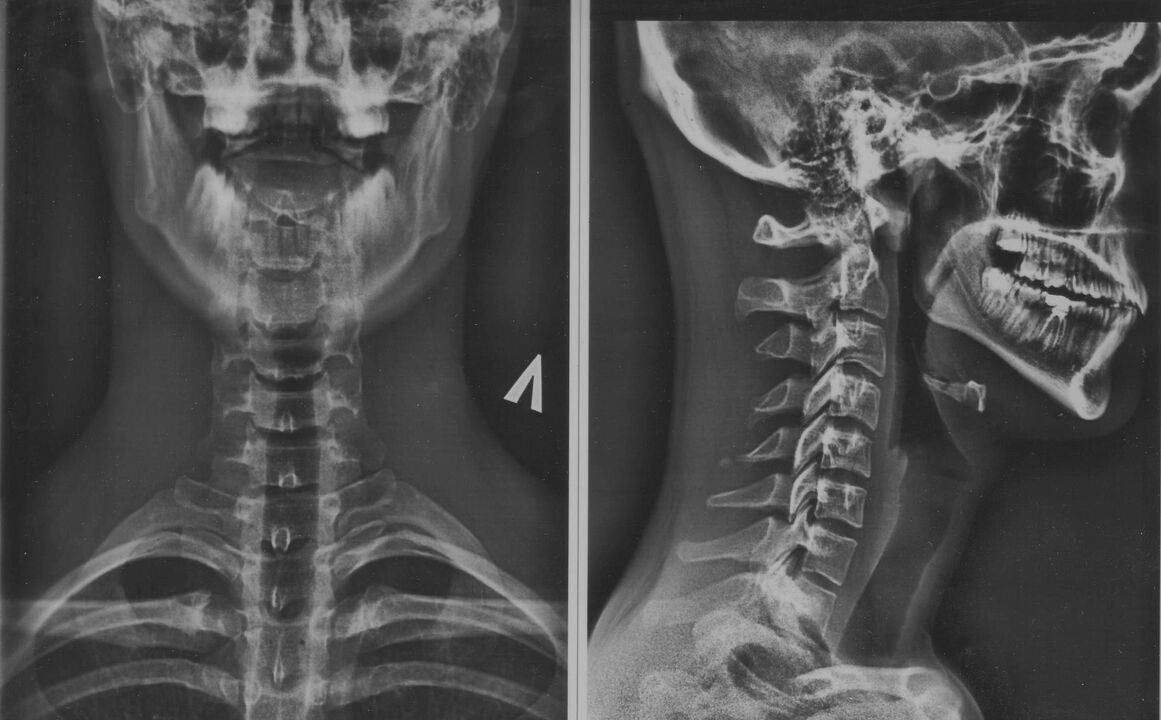
The diagnosis of "osteochondrosis of the cervical spine" is complicated by the low specificity of symptoms and their variety. During the examination, you will need to consult a neurologist, surgeon, orthopedist, cardiologist.
A physical examination is conducted by the doctor by questioning the patient. The main diagnostic burden is on instrumental and laboratory research methods.
- X-ray of the cervical region; At the initial stage of the process, MRI of the cervical region will be more informative - it provides high-quality visualization of hard and soft tissues - it shows the condition of the intervertebral discs, the presence of osteophytes, deformation, damage. nerve roots and blood vessels; assessment of the condition of ligaments, muscles, bone tissue; shows the dynamic state of soft tissues;
- Dopplerography of neck vessels will help to assess hemodynamics and the degree of damage to blood vessels (in particular, the condition of the vertebral artery);
- Contrast myelography - will help suspected disorders of nervous processes;
- ECG and heart echocardiography are used in the differential diagnosis of heart syndrome with cardiovascular diseases.
How to treat cervical osteochondrosis
A complex of therapeutic measures is created taking into account the stage of the disease (acute, chronic), the degree of damage and the causes of the pathology. Use conservative treatment, surgery, mixed approach.
conservative influence
It is a gradual recovery or compensation of the damage against the background of symptomatic treatment. It includes drug therapy, physical therapy, exercise therapy and massage techniques.
medical treatment:
- Painkillers - mainly gels and local ointments; In severe cases - general painkillers in the form of tablets;
- Anti-inflammatory drugs - non-steroidal anti-inflammatory drugs, as well as corticosteroids (short course if necessary);
- Medicines to improve microcirculation and blood circulation in general;
- Chondroprotectors - means of cartilage tissue protection and restoration;
- muscle relaxants - to eliminate muscle cramps and spasms;
- Complexes of vitamins and microelements - necessary for supporting tissues with nutrition and building elements.
Physiotherapy, exercise therapy and self-massage methods are associated with the reduction of acute symptoms.
PhysiotherapyImproves cartilage and bone tissue nutrition. Due to restoration of blood supply to the damaged area. In order to avoid complications, it is recommended to use the method of isometric movements, when instead of actual bending and tilting of the head, which can cause damage, their imitation is used.
Attention!All actions should be taken only after diagnosis and consultation with a doctor.
The technique allows you to develop and strengthen the atrophied short muscles of the neck and stabilize the position of the cervical spine. The sequence of the main exercises:
- Put the palm of your right hand on the side of your head - for 10 seconds, press the palm on your head, and for resistance, stretch the muscles of the head and neck - the head should remain motionless.
- Lower your hand, relax your head and neck muscles for as long as 20 seconds.
- Repeat the exercise with the left hand.
- Place both hands on your forehead with your palms together - press on your forehead for 10 seconds as if you are trying to tilt your head back, while tensing your neck muscles to resist the movement. The head should remain motionless.
- Lower your arms, relax your muscles as much as possible, like the previous exercise.
- Place both hands above the back of your head. By analogy, perform a pressure load on the neck muscles, trying to bend your head forward - it should still be motionless.
- Lower your hands, relax your neck and head muscles. Repeat the set of exercises 4-10 times.
After strengthening the short muscles of the neck, you can start performing dynamic exercises.
Note!Swimming and water aerobics have proven themselves as techniques for restoring cervical mobility.
self massageAllows you to reduce the intensity of local reactions and release muscle clamps during static work. Performance rules:
- Zone of influence - the back of the head, back and side surfaces of the neck;
- carry out the procedure in a sitting position;
- movements should be performed in the direction of the spine;
- Use only your fingers;
- Avoid pressure on the inflamed areas;
- Perform movements smoothly - sharp pressure can cause damage.
PhysiotherapyIt is typical for inpatient treatment and spa rehabilitation. Well proven:
- Electrophoresis - heats the area, improves microcirculation, is used for deep penetration of topical preparations;
- magnetotherapy;
- amplipulse;
- UHF.
Surgical intervention is indicated in complicated extrusion, spinal cord fracture and intractable pain syndromes.
What is dangerous cervical osteochondrosis?
In the neck area is concentrated a dense intertwining of the main blood vessels, nerve processes and dynamic structures of the bone skeleton. In the absence of treatment, serious pathological changes may be observed:
- A weakening of the annulus fibrosus provokes dislocation and subluxation in the area of the most mobile vertebra;
- The presence of osteophytes and muscle spasm leads to disruption of nerve roots and blood vessels, causing compression syndromes;
- Destruction of cartilaginous discs and convergence of vertebrae causes intervertebral hernia with damage to nerve tissue.
Each of these events is followed by a pronounced negative reaction of the whole organism.
Possible complications and consequences
The list of the most common complications of cervical osteochondrosis includes:
- vegetovascular dystonia;
- hypertension;
- oxygen starvation of the brain and its structures;
- Retinal dystrophy with vision impairment;
- malfunction of the thyroid gland;
- Dysfunction of the esophagus and trachea - difficulty swallowing and respiratory spasms;
- unbearable pain in the head, neck, chest, upper limbs;
- Cramps and numbness of the face, hands;
- Disruption of the hypothalamic-pituitary system, which leads to the failure of the entire hormonal activity of the body.
Preventive measures of cervical osteochondrosis
The most effective treatment is disease prevention. Prevention will help you in this. It is enough to follow a few basic recommendations:
- correct your posture
- create a comfortable workplace;
- Take a "Physical Education Minute" break during sedentary work;
- Include in your diet foods rich in calcium, magnesium, phosphorus, silicon - fish, nuts, seeds, legumes, dairy products, fresh vegetables, fruits; limit the intake of salty, sweet, starchy and spicy foods;
- Use an orthopedic mattress and pillow for sleep and rest;
- Engage in non-vigorous sports - it is better to give preference to swimming.
Even if you can't meet all the requirements, moderate exercise, proper nutrition and attention to posture can significantly reduce the risk of developing the condition.
The hidden cause of impotence, male and female infertility is osteochondrosis
Back in school, biology classes tried to convey important information about the huge role of the spine in maintaining human health. Unfortunately, many were busy with more important things and did not understand the words of the teachers. But in vain! Doctors say that disorders of the musculoskeletal system, in particular osteochondrosis, can lead to the development of many serious diseases.
Why osteochondrosis has a strong destructive effect on the human body
Often, men suffer from impotence and infertility, and women try in vain to get pregnant and do not even suspect that this may be caused by ordinary osteochondrosis. It is a fact that the cause of the development of the disease lies in the violation of the blood supply to the spinal tissues and the surrounding muscles. Since there are no blood vessels in the intervertebral discs, they are the first to lack water and other substances. This causes the cartilage to tear, meaning that the discs can no longer absorb the load on the spine. Hence the constant back pain.
If you do not intervene in the process at this stage, then osteochondrosis will continue to progress and cause complications, for example, disc herniation. This, in turn, causes disruption of the segmental apparatus of the spinal cord and disrupts blood circulation, including in the pelvic organs. This is the main reason for the development of many disturbances in the work of internal organs, the impotence and infertility that we are interested in.
The development of impotence in men, in addition to physical disturbances, also contributes to the psychological factor. After all, for every normal, full-fledged man, even one failure in bed becomes a drama, and it does not matter if it is caused by an exacerbation of osteochondrosis, sciatica or other sources of back pain.
Men may experience erectile dysfunction in the presence of cervical or lumbar degenerative disc disease. But in each case, the pathology develops according to its own mechanism.
Cervical osteochondrosis
In the presence of this type of disease, there is a decrease in the quality of blood circulation in the brain, which leads to a violation of the production of sex hormones and substances responsible for vascular tone. Therefore, with cervical osteochondrosis, most often patients complain of decreased sexual desire, anorgasmia and ejaculation problems.
Lumbar osteochondrosis
Since the pelvic area, in particular, the male genital organs are located here, due to disorders in the spinal cord, it is "off" as it turned out, nerve impulses do not always manage to penetrate the genital organs, which leads to erectile dysfunction.
Male and female infertility as a result of osteochondrosis
Often, in the absence of other prerequisites, unsuccessful attempts to conceive a child in both men and women may be the result of pathological processes accompanying osteochondrosis. Most often, the cause of the problem lies not so much in the violation of the blood supply of the organs located in the small pelvis, but in neurological disorders.
Examinations of women suffering from infertility show degenerative changes in the lower part of the chest and in the lower part of the waist. In infertile men, osteochondrosis affects the lumbosacral region. Such differences in the areas affected by osteochondrosis are explained by the peculiarities of the structure and innervation of the pelvic organs in representatives of different sexes.
Sometimes women can't get pregnant even if they don't have any signs of the disease and don't feel the slightest discomfort in the back. This is primarily due to the fact that disorders in the reproductive system can occur even if only the anterior roots of the spinal cord are damaged, which is not accompanied by pain.
Therefore, everyone who is worried about sexual and reproductive function disorders is strongly recommended to undergo the most comprehensive examination of the body, not forgetting the neuropathologist and vertebrologist. Perhaps the root of the problem lies in spine pathologies.


































